What is acupuncture?
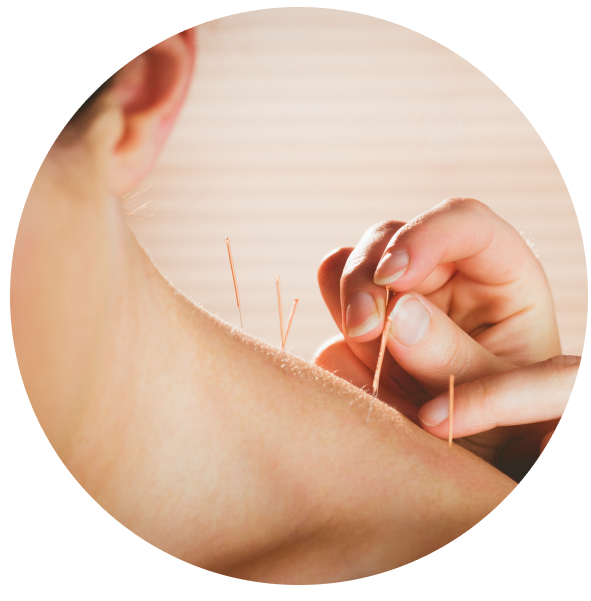
Acupuncture is a wellness technique that originated in China in as early as 6000 BCE. Acupuncture involves a practicition inserting thin needles into different parts of the human bottom. They may move the needles after placement to stimulate the nerves, before leaving them in for a period of time. The needles are commonly removed at the end of the session, but your practitioner may leave in small pressure patches if they consider it necessary.
How much does acupuncture cost?
An acupuncture session will cost a different amount depending on the length of the session and your location. You can expect to pay between $50 and $200 per session depending on the factors above. Some medical insurance plans will cover acupuncture as preventative care, so please speak to your provider about options.
Additionally, acupuncture is offered in many locations via your ClassPass membership, at no additional cost to you.
![[Picture] acupuncture-full [Picture] acupuncture-full](http://images.ctfassets.net/ew96z4wsnz93/5z1VyNgzEErPZCGj631Xqh/781e4490ff5c9e725dcd722ef240d41c/03_Acupuncture_copy.jpg)
What does acupuncture do?
Acupuncture is rooted in wellness practices as a way to improve a person’s energy balance and reduce stress. Acupuncture is often used in medicine as a way to reduce nausea, pain and arthritis. Acupuncture can be done on different body parts, with different varying benefits.
What to wear to an acupuncture session
Comfort is the primary focus of what you should wear to acupuncture. Don’t wear fancy clothes, instead focus on wearing something light and comfortable, so that you can relax. You may be asked to disrobe during acupuncture, so make sure to wear undergarments if that makes you feel more comfortable.
![[Picture] Wellness collage [Picture] Wellness collage](http://images.ctfassets.net/ew96z4wsnz93/siIvDAGQnjQYN1aycW779/b97cbee7f939bfff251b762c565923ff/CRO_Invite-Page_Save-70-Off-Module.webp)